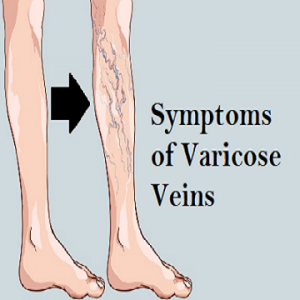
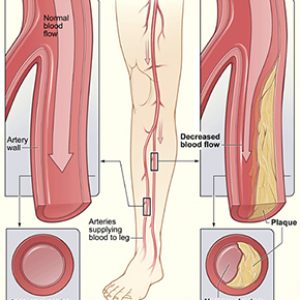
Varicose veins occur when a person’s veins of the leg become swollen and enlarged. In some people, they can cause pain and discomfort while performing daily activities. A range of home treatments may help to reduce the appearance and pain of varicose veins. The doctor may suggest a patient some of the home remedies to be followed for a faster recovery. Around many adults will experience varicose veins at some point in their life. There are several medical treatments for this condition, though a person may also wish to try natural home remedies to relieve their symptoms.
What are varicose veins?
Varicose veins can develop when small valves in the veins start becoming weak. These valves usually stop blood flowing backward through the veins, and when they are damaged blood can accumulate in the veins. This causes twisted and swollen veins that also become visible very easily.
Varicose veins can be noticeable because of their dark blue or purple appearance, sometimes they also often bulge out from underneath the skin.
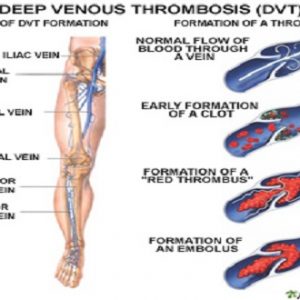
Ten home treatments for varicose veins
1. Exercise
Regular exercise encourages better blood circulation in the legs, which helps to push along the blood that has accumulated in the veins. Exercise also helps to lower a person’s blood pressure, which is another contributing factor to varicose veins treatment.
A small number of exercises help to get the calf muscles working without excessive strain. Effective, low-impact exercises include:
- swimming
- walking
- cycling
- yoga
2. Compression stockings
Compression stockings are available from most pharmacies and can help by applying pressure to the legs. This aids the muscles and veins to move blood toward the heart.
3. Plant extracts
Horse chestnut extract, Aesculus hippocastanum L., may help to reduce leg pain, heaviness, and itching in people with chronic venous insufficiency, which is a major cause of varicose veins. Aesculus hippocastanum L. is available to purchase in health stores and online.
4. Dietary changes
Foods that are high in potassium include:
- almonds and pistachio nuts
- lentils and white beans
- potatoes
- leafy vegetables
- some fish, such as salmon and tuna.
Foods that are high in fiber include:
- nuts, seeds, and legumes
- oats, wheat, and flaxseed
- whole-grain foods.
People who are overweight are more likely to experience varicose veins.
5. Eat more flavonoids
Flavonoids improve blood circulation, which will keep the blood flowing, and make it less likely to pool in the veins. They also help to reduce blood pressure in the arteries and can relax blood vessels, all of which can reduce varicose veins.
Foods that contain flavonoids include:
- vegetables, including onions, bell peppers, spinach, and broccoli
- citrus fruits and grapes, cherries, apples, and blueberries
- cocoa
- garlic
6. Herbal remedies
According to the National Institute of Health, taking grape seed extract, Vitis vinifera orally may help to reduce swelling in the lower legs and other symptoms of chronic venous insufficiency, though there is currently limited evidence for its effectiveness.
7. Choose non-restrictive clothing
Wearing tight-fitting clothes can restrict blood flow. A person may find that their circulation is improved by wearing loose-fitting clothes that do not restrict the blood supply to the lower body.
Wearing flat shoes instead of high heels may also help with varicose veins in the legs.
8. Keep the legs elevated
Keeping the legs elevated, ideally at the same height as the heart or above it will help to improve blood circulation. This reduces the pressure in the leg veins and gravity will help the blood to flow smoothly back to the heart.
9. Massage
Gently massaging the affected areas can help to keep the blood moving throughout the veins. A person can use gentle massage oils or moisturizers for optimal effects.
It is crucial to avoid pressing directly onto the veins, however, as this may damage fragile tissues.
10. Keep moving
Avoid sitting for long periods of time. If a person has to sit for long periods of time for work, they should aim to get up and move around or change positions frequently to keep the blood flowing smoothly.
Avoid sitting with crossed legs, as this can further restrict blood flow to the legs and feet, which may add to circulation problems.
Dr. Advait Kothurkar is a Vascular Surgeon in Pune. He has returned from UK in 2006 and has been practicing in Pune. Being attached to a number of Hospitals in the city as a Vascular Surgeon, he manages all referrals, emergency and elective successfully manage links Bypass Elective and for Trauma.
Panel Consultant for:
1. Sahyadri Specialty Hospital – Karve Road
2. KEM Hospital
3. Deenanath Mangeshkar Hospital
4. Sancheti Hospital
5. Hardikar Hospital
6. Lokmanya Group of Hospital
7. Bharti Vidyapeeth Hospital.
KNOW MORE